Meningococcus (Neisseria meningitis)
Meningococcus bacteria cause several different infections besides meningitis. Meningococi can cause different forms of blood poisoning: septicemia, which is very severe; and meningococcemia, a milder form in which fever may be the only sign of infection. Meningococci can also cause pneumonia, arthritis, and infections of the heart, eye, or other parts of the body.
Meningitis is the most common form of meningococcal infection, accounting for about 75% of cases. Septicemia is the next common – 20% of cases – and the other infections make up the balance. All forms of meningococcal disease are medical emergencies and require immediate medical attention. Prompt diagnosis and treatment with antibiotics improves the change of a good outcome without complications. Septicemia is more dire. Less than one in twenty people die of meningococcal meningitis. Four to 8 in twenty die of septicemia. If shock – low blood pressure and blood circulation failure – occurs before treatment can be started, the death rate from meningococcal septicemia is more than twelve in twenty, or 60%.
The next most common group to be infected is teens and young adults from 15 to 24 years. After the age of 25, most people have developed a natural immunity and the annual rate of disease is one tenth that in infants. Most cases occur between December and April.

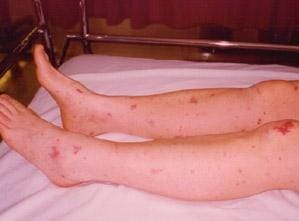
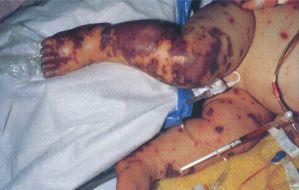
A person with meningococcal septicemia will not likely have a headache, stiff neck, or neck pain. Septicemia infections almost always result in a rash; meningitis infection will sometimes cause a rash but not always. The rash, consisting of red spots or bruises, may appear anywhere on the body and may not develop until the disease is quite advanced. It is the most specific and most noticeable symptom of meningococcal septicemia, primarily because it does not fade under pressure.
To check for meningococcal rash, press the side of a colorless glass against the rash. If the redness does not fade with the pressure, the rash is likely meningococcal. Note that the redness may fade under pressure when the rash first appears, so it is wise to do the glass test more than once.
| Meningococcal Infection Symptoms | Meningitis | Septicemia |
|---|---|---|
| Fever, usually high | yes | yes |
| Cold hands and feet | yes | yes |
| Drowsiness, impaired consciousness | yes | yes |
| Irritability, fussiness, agitation | yes | yes |
| Severe headache | yes | yes |
| Vomiting | yes | yes |
| Stiff neck | yes | no |
| Pain on moving neck | yes | no |
| Rash | not always | yes |
| Rapid breathing | rarely | yes |
| Pain in muscles and legs | rarely | yes |
Meningococcal bacteria spread through direct contact with secretions from the nose and throat of a person who is a carrier of the meningococcus. A carrier is a person who has the meningococci living on the surface of the lining of the nose and throat without having any symptoms or becoming ill. About 10 to 20 per cent of adolescents and adults carry the meningococcus bacteria in the back of their noses and throats, they are carrier who can spread the bacteria to others. These carrier infections may last up to six months or more.
Because the bacteria are fragile outside the body, spread from an infected carrier to another person requires close, direct physical contact through kissing, coughing or sneezing. The bacteria also spread through saliva. Sharing anything that comes in contact with the mouth can spread the bacteria from person to person – mouthpieces on musical instruments, drinking glasses, lipstick, eating utensils, toys and such can all spread the bacteria.
A sick person can spread the disease up to seven days before becoming ill and for one day after antibiotic treatment begins. Most illnesses are the result of contact with a healthy carrier rather than someone who is sick with meningococcal disease. Treatment is with antibiotics, usually penicillin. Other antibiotics may be given to protect individuals who have had contact with a case of meningococcal disease. There are effective vaccines to protect against most kinds of meningococcal disease.
